Bracing for 10 million AMR deaths per year by 2050
February 01, 2024 | Thursday | Views | By Vivek Padgaonkar, Former Director, OPPI; and Dr Hari Natarajan, Founder & Managing Partner, Pronto Consult
Antibiotic resistance is intrinsically linked to animal and human consumption patterns, partly driven by inappropriate use of antibiotics. In turn, the emergence of antibiotic resistance fuels changes in consumption patterns, as more costly broad-spectrum antibiotics become required to manage even common conditions.
Variations exist between Indian states in terms of their population age structure, health-seeking behaviour, infectious disease burden, health systems organisation and the relative contribution of the public and private sectors in healthcare
The rapid emergence of resistant bacteria is occurring worldwide, endangering the efficacy of antibiotics, which have transformed medicine and saved millions of lives. Many decades after the first patients were treated with antibiotics, bacterial infections have again become a threat. The antibiotic resistance crisis has been attributed to the abuse, overuse and misuse of these medications, as well as a lack of new drug development by the pharmaceutical industry due to reduced economic incentives and challenging regulatory requirements.
In Asia, infectious diseases make up a substantial 40 per cent of the total disease burden. This includes formidable illnesses like Malaria, Tuberculosis (TB), and Human Immunodeficiency Virus (HIV), which necessitate treatment with antibiotics. Unfortunately, in India, there is a lack of a robust surveillance system. When it comes to Malaria, the conventional treatment with Chloroquine has proven ineffective, thereby requiring the use of more costly artemisinin derivatives. Shockingly, 28 per cent of TB cases in the region are classified as Multi-Drug Resistant (MDR) TB. Moreover, second-line therapy for managing HIV is six times more expensive. This not only makes the fight against these diseases more challenging, but it also significantly escalates the associated costs.
In a recent study conducted by the Indian Council of Medical Research (ICMR), alarming revelations about Antibiotic resistance have emerged, painting a grim picture of healthcare in India. The abuse and overuse of antimicrobials, including antibiotics, antivirals, and antifungals, have led to widespread resistance to these drugs within the community
The battle against antibiotic resistance is a critical one, demanding a collective effort from healthcare professionals, researchers, and policymakers alike.
Antibiotic development
Antibiotic development is no longer considered to be an economically wise investment for the pharmaceutical industry. Because antibiotics are used for relatively short periods and are often curative, antibiotics are not as profitable as drugs that treat chronic conditions, such as cardiac, diabetes, psychiatric disorders, asthma, or gastroesophageal reflux. A cost–benefit analysis by the Office of Health Economics in London calculated that the net present value (NPV) of a new antibiotic is only about $50 million, compared to approximately $1 billion for a drug used to treat neuromuscular disease. Because medicines for chronic conditions are more profitable, pharmaceutical companies prefer to invest in them. Over 80 years, a total of 150 antibiotics have been developed. However, it is not anticipated that any new antibiotics will be introduced for a minimum of 10 years.
Because of these factors, many large pharmaceutical companies fear a potential lack of return on the investment that would be required to develop a new antibiotic. The Infectious Diseases Society of America (IDSA) reported that as of 2013, very few antibacterial compounds were in phase 2 or 3 development.
Co-trimoxazole clinical effectiveness
Clinical Effectiveness comparison of Co-trimoxazole versus leading antibiotic molecules and against leading diseases conclusively proves that this most economical molecule ie Co-trimoxazole is considered the antimicrobial agent of choice in the treatment of many diseases, minimising the risk of vital organ involvement and relapses and is superior or equal to many molecules that are prescribed in the country.
Therapeutic Substitutes in Antibiotics
In India, out-of-pocket expenditure constitutes ~60 per cent of total health expenditure with a substantial 40 per cent being incurred on medicines (Report of Standing National Committee on Medicine SNCM 2022). With this background, it is of paramount importance that the accessibility and availability of essential medicines be enhanced to reduce the financial burden.
The National List of Essential Medicines (NLEM) of the Ministry of Health & Family Welfare (MoH&FW) is incorporated in the Schedule-I of the Drugs (Prices Control) Order, 2013 (DPCO, 2013). The formulations under Schedule-I of DPCO, 2013 are mentioned according to their therapeutic category. There is no separate classification of antibiotics based on the generations i.e., 3rd or 4th generation Antibiotics. However, Section 6.2 of Schedule-I of DPCO, 2013 deals with the class, “Antibacterials”, which includes 95 formulations of 27 medicines. Out of these, ceiling prices for 74 formulations have been fixed under NLEM 2022 and 11 formulations under NLEM 2015 as of July 31, 2023, by the National Pharmaceutical Pricing Authority (NPPA).
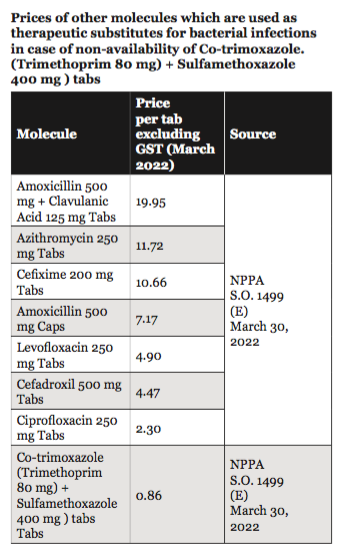
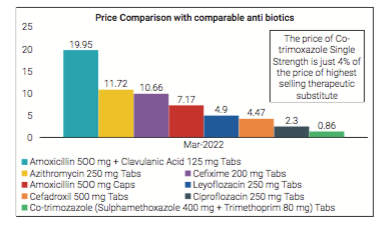
As evidenced by the data, despite the seemingly strong generic competition, gauged in terms of the number of players present in each of the therapeutic areas and at the level of formulations/molecules, consumers in India ostensibly pay a premium for brands.
The substantially large price variations amongst various brands cater for the same therapeutic areas. (CCI Nov 18, 2021, mentions about the same formulations).

The average number of brands per formulation across therapy areas hides the stark variation observed within each formulation. The number of brands varies considerably even between different strengths and doses.
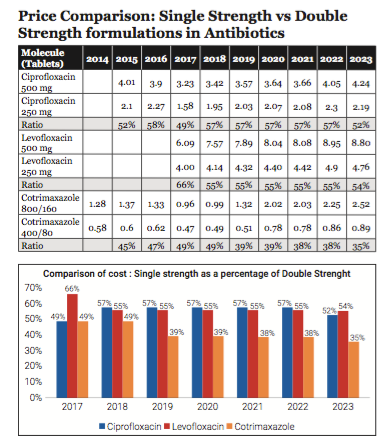
The difference in costing of the single strength and double strength is usually attributed to the quantum of API, whereas the rest of the cost components such as excipients and packaging costs are similar, therefore in terms of costing, the cost of single strength is usually more than 50 per cent of double strength. A similar difference can be observed in the prices in the above table which exemplifies that the ratio of the price of single strength as a percentage of double strength is over 50 per cent for antibiotics like levofloxacin and Ciprofloxacin, whereas for cotrimoxazole it is as low as 35 per cent.
The relatively larger number of brands are typically present in markets with a larger number of formulations. In some therapy areas, the number of brands created is disproportionately larger than the number of formulations.
The market failure (non-availability of medicines in the market) with respect to pharmaceuticals in the context of India can be attributed to several factors, but the main reason is that the demand for medicines is largely prescription driven and the patient has very little choice in this regard. The sales promotion drives doctors’ prescriptions. The sales promotion budget is a function of the revenue generated by the brand.
Co-trimoxazole (Trimethoprim 80 mg+Sulfamethoxazole 400 mg ) tabs proved to be significantly lower in price to the patients, with fewer options than any of the above-mentioned therapeutic substitutes for patients suffering from bacterial infections.
Unfortunately, if the financial unviability continues, companies marketing Co-trimoxazole may be left with no option but to exit from this category leaving ailing patients with many costly exploitative options.
AMR & Health Care Professionals (HCPs)
In the latest study which was conducted amongst 763 HCPs across India including Metros and Class I, II towns and beyond. All of the HCPs opined that AMR is something that they are aware of in their clinical practice. Medical practitioners recognise that AMR is a global health threat and poses a significant challenge to their ability to treat infections effectively, which can lead to higher mortality rates and longer hospital stays.
In the 1436 bills from the chemist's shops across the country analysed in another research study, it was observed that patients buy some antibiotic or the other, in 63 per cent there was one or more antibiotics present.
One of the medical practitioners mentioned, “Antibiotics are less effective when used repeatedly and without any control. We have seen more than 50 per cent of cases wherein repeated usage of Antibiotics has resulted in AMR in our patients and we are very concerned with the same in India.”
Answering the Query whether they feel pressured to prescribe antibiotics even when they suspect they may not be necessary, HCPs mentioned that patients pressurise them to prescribe an antibiotic as they feel that the antibiotic will provide quick relief and they can get back to work faster. The medical practitioners said that they believe in the importance of educating patients about antibiotics and they spend time explaining to their patients when antibiotics are necessary and when they are not.
When Pronto Consult conducted a study amongst 456 chemist shops on the key question of “How often do you encounter patients requesting antibiotics for conditions that do not typically require them?”, almost 73 per cent of the chemists revealed that patients directly ask them for an antibiotic and want to buy. Most of them don’t have a doctor’s prescription and want to buy an antibiotic, maybe a formulation of Amoxy-Clav, Azithromycin or Cefixime.
Pronto Consult also spoke with 874 consumers on their awareness of Antimicrobial Resistance. 71 per cent were not aware of AMR while 29 per cent said they have heard or read in the news. This is a serious concern which needs to be addressed by proper education and needs to be taken up by all stakeholders.
A reply to a question posed to consumers, “Do you pop an antibiotic every time you are ill?”, 81 per cent mentioned they have taken antibiotics most of the time they have fallen ill and 71 per cent stop the medicine as soon as they feel fine without completing the full prescribed course of the antibiotic.
Dr Karishma Shah, Founder, Pronto Consult said, “Doctors generally view AMR as a complex and critical issue that requires a multifaceted approach, including responsible antibiotic prescribing, patient education, research, and collaboration among healthcare professionals and policymakers to combat this growing threat to public health.”
Karishma adds "Antimicrobial Resistance reminds us that in the battle between man and microbe, adaptability is the true measure of strength. It's a call to action for responsible stewardship of antibiotics and the pursuit of innovative solutions, as our survival depends on the wisdom to evolve with the ever-changing microbial world."
Government’s initiatives on AMR
The Government has taken cognisance of the increasing issue of Antimicrobial Resistance (AMR) which can be one of the public health crises in coming years and has taken the following initiatives planned to prevent the increasing risk of AMR;
The Government is planning to expand and diversify the AMR National Action Plans (NAPs) with the robust surveillance systems that will be followed in the hospitals to facilitate early detection of AMR. The centre is aware of the challenges posed by AMR in India. It is a multifaceted problem with significant consequences for individuals as well as Health Care Systems. To capture the trends and patterns of AMR in India, ICMR has established an AMR surveillance and research network (AMRSN) to monitor data on the trends and patterns of antimicrobial resistance of clinically important bacteria and fungi limited to human health from 30 tertiary hospitals.
The MoH&FW has taken several steps to address the issue of AMR including:
- AMR surveillance network has been strengthened by establishing labs in State Medical Colleges. 38 sites in 30 States/UTs have been included in this network so far.
- A national action plan for containment of Antimicrobial Resistance (NAP-AMR) focusing on the One Health approach was launched in April 2017 to involve various stakeholder ministries/ departments. Delhi Declaration on AMR– an interministerial consensus was signed by the ministers of the concerned ministries pledging their support in AMR containment.
- AMR Surveillance Network: ICMR has established an AMR surveillance and research network (AMRSN) comprising 30 tertiary care hospitals, both private and government, to generate evidence and capture trends and patterns of drug-resistant infections in the country.
- AMR Research & International Collaboration: ICMR has taken initiatives to develop new drugs/medicines through international collaborations to strengthen medical research in AMR. Further, to create awareness IEC materials including audio, videos, social media messages and Outdoor Media have been developed and are also shared with states for further dissemination. MoHFW released the National Guidelines for Infection Prevention and Control in Healthcare Facilities in January 2020.
The National Centre for Disease Control under MoHFW is conducting several stakeholder consultations to monitor the implementation of the existing National action plan on AMR by various departments and ministries. The consultations are also to guide the development of a more practical and implementable National action plan on AMR 2.0.
Under the National Programme on AMR Containment, 38 state medical colleges/large Government hospitals in 30 states/UTs have been strengthened to do AMR surveillance on 7 priority pathogens. These sites have robust surveillance systems to facilitate early detection of AMR. AMR emerging alerts are also confirmed at the National Reference Laboratory.
Threat to humanity
The impact of loss of antibiotic efficacy due to the emergence of drug resistance in various bacterial pathogens is creating a ´silent pandemic’.
AMR poses a substantial threat to humanity, with the potential to render some of our most innovative medicines ineffective against common infections that for decades, and in some cases over a century, have been easily managed with antibiotics.
With the potential for AMR to push 28 million people into poverty and 10 million deaths/year by 2050 (especially in countries), the time to invest in solutions is now. As per the latest estimates for 2021, AMR-related deaths were already more than 4 million.
The global response does not match the scale of the problem. The market for new antibiotics is nearly non-existent and, as a result, more than 82 per cent of all antibiotic approvals occurred before the year 2000.
The Supreme Court of India vide Order dated 12.11.2002 in SLP no. 3668/2003 (Union of India vs K.S. Gopinath & others) has directed the Government to ensure that essential and life-saving drugs should be available & affordable to the common public.
The market failure alone may not constitute sufficient grounds for government intervention, but when such failure is considered in the context of the essential role pharmaceuticals play in the area of public health, which is a social right, such intervention becomes necessary, especially when exploitative pricing for the therapeutic substitutes makes medicines unaffordable and beyond the reach of most and also puts huge financial burden in terms of out-of-pocket expenditure on healthcare.
The continuous price control has led to financial unviability therefore causing an erosion in the value of Co-trimoxazole (Trimethoprim 80 mg+ Sulfamethoxazole 400 mg) from 2013 to 2023 ~ 84 per cent erosion of value.
A collective responsibility
The government should make the availability of drugs at affordable prices while ensuring affordability, accessibility cannot be jeopardised and the lifesaving essential medicines must remain available to the general public at all times. Therefore, the government needs to take the considered view that the financial unviability of these formulations -Co-trimoxazole (Trimethoprim 80 mg+ Sulfamethoxazole 400 mg)tabs should not lead to a situation, where these drugs become unavailable in the market and the ailing patients are forced unfortunately to switch to very costly alternatives and therapeutic substitutes heavily promoted from the non-scheduled formulations category.
AMR is a silent pandemic, a reminder that our actions today shape the future of medicine. To preserve the power of antibiotics, we must act responsibly and collectively, for a world where infections remain treatable and lives are safeguarded.













